Find care now
If you are experiencing a medical emergency, please call 911 or seek care at an emergency room.
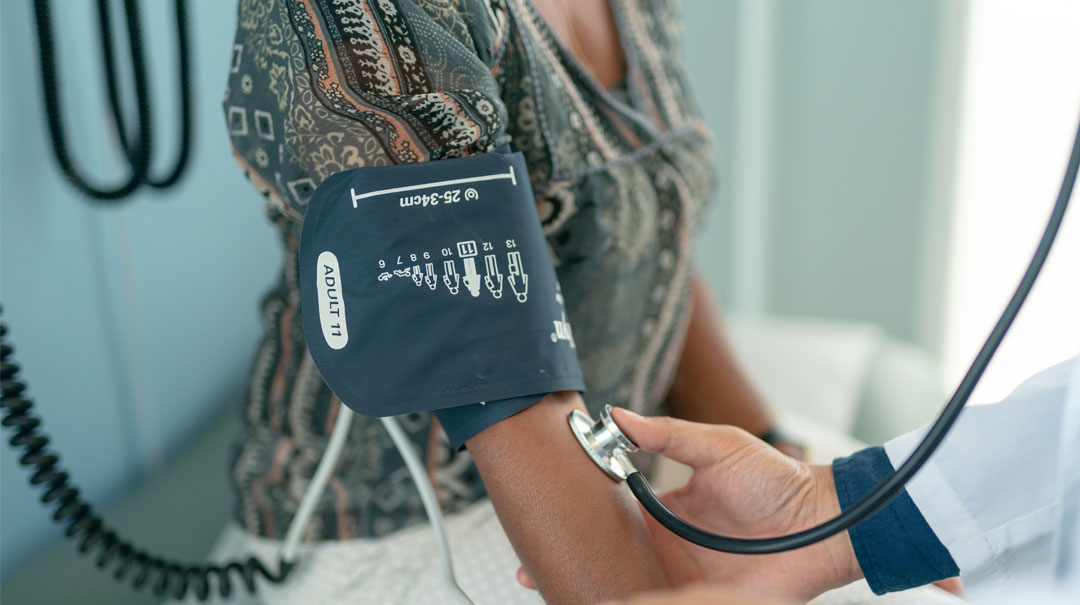
But with each passing week, we’ve come to understand more about what makes the novel coronavirus tick. We haven’t learned everything, but time, experience, and research have unlocked many of its secrets and behaviors, as we pursue new treatment and prevention strategies.
At this stage of managing the virus, we can confirm that cardiovascular disease in general presents a known risk for complications and adverse outcomes. But hypertension alone does not.
Elevated blood pressure plays a role if coupled with other cardiovascular diseases, like coronary artery disease, congestive heart failure, and heart attack—and it tends to affect older people. So, it’s together with these other factors that high blood pressure may become more dangerous for someone who contracts the virus.
Don’t Avoid the Hospital
Because we’re increasingly aware of the risks—and because cardiac disease exists in most communities—we continue to recommend that patients with cardiac illness be extra-vigilant about their health. Take all the precautions to prevent infection, like social distancing, limiting exposure to others, wearing a mask when out in public, and frequent handwashing.
The new virus targets the respiratory system—which, in many cases, is already compromised in those with cardiovascular illness. We don’t see evidence that cardiovascular disease patients are more likely to contract the virus, except those with compromised immune systems. But we do know that people with heart disease fare an average two to three times worse with COVID-19 than those without heart disease. The multitude of issues just makes it more difficult for the body to weather the infection storm.
So, getting the cardiovascular care you need is as important as ever, and there’s no reason to stop your ongoing treatment. This is not the time to avoid the doctor or hospital for fear of a virus—especially if you experience signs of a heart attack.
We know “COVID phobia” is real. Medical centers have experienced significant reductions in patient volume since stay-at-home orders went into effect. But I can’t stress this enough: if you need medical attention, even routine monitoring or checkups, you have options. A MedStar Video Visit, for example, is a great way to stay in touch with your cardiologist, without leaving home.
If you do need to be seen, visiting a MedStar Health facility is as safe as it’s ever been. We take every possible precaution to protect both patient and practitioner—limiting exposure, using protective equipment, monitoring temperatures, and isolating infected persons.
In fact, since the beginning of March, MedStar Heart & Vascular Institute has performed 11 heart transplants and 20 artificial heart procedures, without a single problem or complication related to the virus. We continue to provide the highest level of care for those who need it, safely and reliably.
Every day, cardiologists know more about how COVID-19 interacts with cardiovascular diseases. @TaylorMHVICard covers the latest developments. https://bit.ly/3cfwUpi via @MedStarWHC
Click to Tweet
Coronavirus and Blood Pressure
We know COVID-19 latches onto receptors in cells that trigger the vessels to regulate blood pressure. These same receptors are the target of some of the more popular blood pressure medications: ACE inhibitors such as benazepril, enalapril, lisinopril, and ramipril, as well as angiotensin receptor blockers (ARBs), including candesartan, irbesartan, olmesartan, and valsartan.
That has caused people to wonder if they should stop taking their medications. The answer is almost always “NO.” Any evidence showing that medications make the virus worse is both sparse and speculative. The risks of elevated blood pressure are far greater and well known—so it’s never a good idea to stop your medications.
Naturally, if you’re concerned, have a conversation with your doctor to determine the best course of action.
There is also some evidence indicating that some blood pressure medications might actually help protect against the virus. We don’t know all the details yet, but studies are underway to shed more light on potential effects.
Other Cardiac Issues
Most of the other cardiac problems we see associated with this condition are not a complete surprise. We see similar issues in severe cases of flu and other viral infections. For example, when the body mounts an immune defense against any invader, the heart and blood vessels register stress. That can increase the risk of heart attack, make symptoms of heart failure worse, and sometimes weaken the heart muscle.
Although the new pathogen is creating some unique problems, we see less impact on heart patients than we first expected. However, the virus can mimic heart attack, even in people without compromised cardiac blood flow. It causes unusual blood clotting which can affect the heart and its network of blood vessels. This may be the cause of heart damage observed in a very small percentage of victims—and it can be picked up with blood tests.
There’s still a lot we don’t know but the science is advancing rapidly, and every cardiac patient affected by the virus increases our knowledge as we move toward reliable treatments and a potential vaccine.
Heart Disease Doesn’t Wait
We know many people are staying away from healthcare thanks to fear of the virus. But heart disease won’t wait for this pandemic to end. The MedStar Heart & Vascular Institute team is doing everything possible to keep the community healthy, providing front-line care for cardiovascular disease at all levels.
Now, more than ever, it’s a time to be vigilant. Coronavirus is a triple-edged sword. It can create some heart disease; make existing disease more serious; and may keep people with disease away from the care they truly need.
Turn to Telehealth
But one big silver lining is the dramatic progress of telehealth, removing roadblocks between patient and physician. This new crisis has prompted regulators and insurance companies to relax restrictions on remote care and gives providers and patients countless opportunities to streamline and improve the process. In fact, we currently conduct as many as 90 percent of outpatient visits remotely.
To get the most out of your MedStar Video Visit, make the appointment! Telehealth is easy, convenient, and brings the benefit of interacting face-to-face with practitioners who care deeply about your well-being. You can have a friend or loved one by your side to help take notes and answer the doctor’s questions. You can even include a loved one from a distance, something nearly impossible with a traditional office visit.
If you have a blood pressure monitor, keep track of your pressure a few days before the video visit. This is valuable information for the cardiologist. Have your medications handy: we typically do a full medication review on each call, and you can save time by assembling them beforehand. Write down all your questions before the visit, to make them easier to remember.
Although this virtual visit isn’t a traditional physical exam, we learn a lot by observing how you look and sound and by asking the right questions. Answer those questions honestly. Be sure you have a good Internet connection and a reliable video device with a charged battery. We like smartphones since they can be easily pointed around when it comes time to look at your medications, your extremities, or other indicators. If you need help, consider recruiting a family member with technical skills. Keep pen and paper handy to write down any new instructions.
Beyond the convenience, telehealth visits are proving to be a very positive experience for both patients and providers. We miss seeing you…and technology provides the next best thing. Another benefit: because it removes the distractions of travel, the waiting room and the busy office, we can focus on what matters most, a meaningful conversation about your health.
Remember, in an age of elevated infection risk, keeping your heart healthy is more important than ever. It’s up to you to do the right thing. Stay on your medications. Keep an open dialogue with your doctor, that’s why we’re here. And if you feel something isn’t quite right, don’t delay, report it right away.














