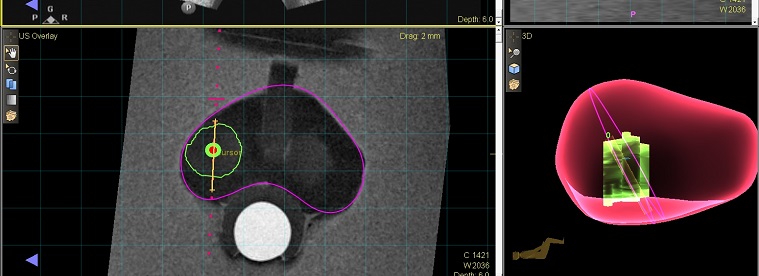
Left Image: The target from an MRI is merged with an ultrasound image for targeting. Right Image: The biopsy locations are captured by the MRI-Ultrasound fusion technology.
Ideally, doctors would catch every case of prostate cancer early, before it has time to grow and spread. Early detection gives men more options, whether that involves treatment or active surveillance to make sure the cancer doesn’t continue to develop.
But standard approaches can’t always locate the prostate cancer. That’s an issue for many of my patients. One man had previously had five standard biopsies, all of which were negative for prostate cancer. But he still had high levels of PSA, or prostate-specific antigen, which is a potential indicator of prostate cancer. I told him, “You really should get an MRI.”
The patient’s MRI (magnetic resonance imaging) test showed there was an abnormality in an area of the prostate where we don’t usually see tumors—one that’s difficult for us to access during a standard biopsy. So we used an advanced technique called an MRI/ultrasound fusion biopsy, which uses both MRI and ultrasound, to help detect this patient’s prostate cancer.
This patient would not have been diagnosed as early as he was without having an MRI/ultrasound fusion biopsy. And this is just one of the many examples I’ve seen of this technology’s value to patients.
The benefits of MRI/ultrasound fusion biopsy
Prostate cancer is a serious problem, both nationwide and in the Washington, D.C., area. Locally, we have a prostate cancer incidence rate of 120.1 men per 100,000. That means more than 120 men out of every 100,000 in the area have prostate cancer—a rate that’s nearly 18 percent higher than the national average.
I recommend a prostate biopsy for men who repeatedly have test results that show high PSA levels. We traditionally use an ultrasound probe to first see if there are any abnormal areas in the prostate. If there are, we target the biopsy in those areas. If there aren’t, we sample 12 random areas to see if we can locate any cancerous cells. The challenge with this approach is that it’s possible to still miss cancerous cells.
As we’ve begun to use MRI scans more often, we’re able to find tumors within the prostate. MRI scans are especially helpful for detecting aggressive prostate tumors. Many times, I see patients who have high PSA scores but negative biopsies, and prostate tumors show up on an MRI scan.
MRI/ultrasound fusion biopsy combines the best parts of MRI and ultrasound for prostate biopsies. The fusion approach starts with an MRI scan of the prostate. We then use that to guide us as we perform an ultrasound and biopsy at the same time. Merging these images is almost like having a homing device in the prostate, telling us to change angles or move our probe slightly.